
How is Impetigo Transmitted?
Impetigo is a highly contagious skin infection that affects millions of people worldwide each year. Bacteria, primarily Staphylococcus aureus and Streptococcus pyogenes, cause red sores, blisters, and a characteristic honey-colored crust on the skin. Understanding the transmission of impetigo is crucial to prevent its spread, especially among vulnerable populations such as children, wrestlers, and other athletes in close contact. This blog aims to shed light on the modes of transmission of impetigo, delve into its symptoms, and explore preventive measures to protect ourselves and our loved ones from this skin condition.
Understanding Impetigo & How It's Transmitted
Definition and Types of Impetigo
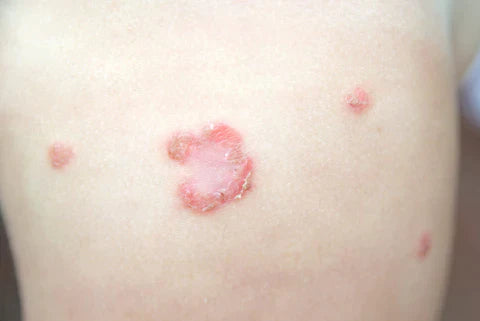
Impetigo is divided into three main types, each with distinct characteristics and severity levels. Non-bullous impetigo is the most common form, characterized by small blisters that quickly burst to leave a yellowish crust. Bullous impetigo involves larger blisters filled with a clear fluid that forms on unbroken skin, primarily in infants and young children. Ecthyma, the most severe form, penetrates deeper into the skin, causing painful ulcers. Recognizing these types is the first step in understanding how impetigo is transmitted and subsequently managed.
Common Symptoms and Signs to Look Out For
Regardless of the type, impetigo symptoms usually include red sores or blisters that burst, ooze for a few days, and then form a yellow-brown crust. The sores can be itchy and may be painful. Swollen lymph nodes near the infection site can also occur. Early detection and treatment are essential to prevent the spread of the infection to others and to other parts of the body.
The Demographics Most Affected by Impetigo
Impetigo predominantly affects children, particularly those between 2 and 5 years of age, due to their developing immune systems and close contact in settings like schools and daycare centers. However, athletes, especially wrestlers, are also at high risk due to the nature of their sport, which involves extensive skin-to-skin contact. Understanding how impetigo is transmitted in these close-contact environments is key to implementing effective preventive measures.
This introduction and overview set the stage for a deeper dive into the transmission of impetigo. Highlighting the importance of knowledge and prevention in managing this common yet preventable skin condition. By focusing on the specific ways impetigo spreads, who is most at risk, and the primary symptoms to watch for, this blog aims to equip readers with the necessary information to prevent the spread of impetigo in their communities.
Key Modes of How Impetigo is Transmitted

Understanding how impetigo is transmitted is crucial for preventing its spread. This contagious skin infection primarily spreads through two modes of contact: direct and indirect. Additionally, environmental factors play a significant role in its transmission dynamics.
Direct Contact
The primary way how impetigo is transmitted is through direct skin-to-skin contact with an infected individual. When the bacteria from the sores or blisters of an infected person come into contact with another person's skin, especially if there are cuts, scratches, or eczema, it can easily spread. Wrestlers and athletes are particularly at risk due to the constant close contact inherent in their sports. Making them more susceptible to acquiring and spreading the infection.
Indirect Contact
Indirect transmission happens when a person touches objects or surfaces contaminated with bacteria from an infected individual. Common items include towels, clothing, bedding, toys, or sports equipment. This mode of transmission highlights the need for personal hygiene and caution in shared spaces, especially in communal living areas and locker rooms where people frequently exchange such items.
Droplet Transmission
Although less common, droplet transmission is another potential route for how impetigo is transmitted. This can occur when an infected person coughs or sneezes, and the respiratory droplets come into contact with another person's skin or mucous membranes. This mode highlights the importance of respiratory hygiene in preventing not just impetigo but other infectious diseases as well.
Environmental Factors
The bacteria that cause impetigo thrive in warm, humid conditions. Summer months often see a spike in impetigo cases, particularly in environments that foster close contact and shared equipment or facilities. Recognizing and mitigating these environmental factors are key steps in controlling the spread of impetigo.
The Role of Bacteria
The Role Bacteria Plays in The Transmission of Impetigo
A deeper understanding of the bacteria responsible for impetigo, Staphylococcus aureus and Streptococcus pyogenes, reveals why it's a prevalent skin infection and how its transmission can be curtailed.
Bacteria Responsible
Staphylococcus aureus and Streptococcus pyogenes are the main bacteria responsible for impetigo. These bacteria can live harmlessly on the skin until they enter through a cut or lesion. Once inside, they cause the symptoms associated with impetigo, such as sores and blisters. These bacteria are particularly adept at exploiting small breaches in the skin's defense, leading to rapid spread and infection.
How These Bacteria Infect Skin and Cause Symptoms
The infection process begins when the bacteria penetrate the skin's outer layer, leading to inflammation and the development of sores. The body's immune response to these bacteria can cause symptoms to appear rapidly. The toxins produced by these bacteria can also lead to the formation of blisters and the characteristic crusty sores of impetigo.
Bacterial Carriers and Asymptomatic Transmission
Bacterial carriers — individuals who carry the bacteria without showing any symptoms themselves — play an important role in the transmission of impetigo. These carriers can unwittingly spread the bacteria to others, highlighting the challenge in controlling impetigo outbreaks. Asymptomatic transmission underscores the importance of universal hygiene practices, even among individuals who appear healthy, to prevent the spread of impetigo.
This section emphasizes the importance of understanding the bacterial mechanisms behind impetigo and the varied ways through which it can spread. By recognizing the role of direct and indirect contact, environmental conditions, and the characteristics of the bacteria involved, individuals and communities can take informed steps to prevent the transmission of this highly contagious skin infection.
High-Risk Groups: Who is Most Affected by How Impetigo is Transmitted
Understanding the transmission of impetigo helps clearly identify the groups and settings most vulnerable to outbreaks, enabling more effective targeting of preventive measures.
Identifying Who is Most at Risk
The primary groups at risk for impetigo include children, particularly those between the ages of 2 and 5, due to their close contact in schools and daycare centers. Athletes, wrestlers, and military personnel also fall into the high-risk category because of their frequent skin-to-skin contact and shared living or training environments. These groups are more susceptible not only to contracting impetigo but also to facilitating its spread.
Settings Prone to Outbreaks
Settings that foster close contact and shared use of items are particularly prone to impetigo outbreaks. Schools, daycare centers, gyms, and locker rooms can become hotspots if preventive measures are not diligently practiced. Wrestling mats and sports equipment used by teams present a significant risk if not properly disinfected between uses. Recognizing these settings as potential transmission vectors is crucial for controlling outbreaks.
The Impact of Skin Conditions and Injuries on Transmission Risk
The presence of cuts, scratches, or any break in the skin significantly increases the risk of transmitting impetigo. Skin conditions such as eczema or dermatitis can also heighten susceptibility because they compromise the skin's barrier function. Individuals with these conditions need to be particularly vigilant in environments where impetigo transmission risk is high.
Preventing the Spread: Measures to Block How Impetigo is Transmitted

Prevention is key to controlling how impetigo is transmitted. Implementing effective hygiene practices and taking specific measures can significantly reduce the risk of spreading this infection.
Hygiene Practices
Regular hand washing and bathing are fundamental in preventing impetigo. It's crucial to educate high-risk groups, especially children, on the importance of hygiene. Avoiding the sharing of personal items such as towels, clothing, and sports equipment is also critical. For athletes and those in constant physical contact, using antibacterial body wipes before and after activities can offer additional protection.
Disinfection Measures
To minimize the risk in communal settings like gyms and schools, use matguard surface wipes and surface sprays to disinfect areas that come into frequent contact with skin. Regular disinfection of sports equipment, wrestling mats, and other surfaces can significantly reduce the transmission of impetigo bacteria.
Measures for Households with Impetigo Cases
If someone in your household is diagnosed with impetigo, isolate their personal items and ensure they follow strict hygiene practices. Covering wounds and lesions helps contain the bacteria and prevent its spread to household members and surfaces.
Seeking Medical Advice and Antibiotic Use
At the first sign of impetigo, seek medical advice. Early diagnosis and treatment with antibiotics can halt the spread of infection. Healthcare providers can advise on the best treatment course, including whether topical or oral antibiotics are necessary. Completing the full course of antibiotics as prescribed is crucial to fully resolve the infection and prevent resistance.
Adhering to these preventive measures can drastically reduce the risk of impetigo transmission. Educating people about the transmission of impetigo and actively engaging in hygiene and disinfection practices protect high-risk groups and prevent outbreaks in vulnerable settings.
Diagnosis and Treatment
Treatment Options for Those Who Transmitted Impetigo
Understanding the diagnosis and treatment of impetigo is crucial for controlling its spread and effectively managing the condition. This section explores the methods healthcare professionals use to diagnose impetigo and the treatment options available to those affected.
Overview of How Impetigo is Diagnosed
Impetigo is primarily diagnosed through visual inspection by a healthcare provider. The distinctive appearance of the sores and blisters typically allows for a straightforward diagnosis. In cases where the diagnosis is uncertain, or if the infection does not respond to initial treatment, a culture test may be performed. This involves taking a sample from the sores to identify the specific bacteria causing the infection, which helps tailor the treatment plan.
Treatment Options
Treatment for impetigo aims to accelerate healing, improve comfort, and prevent the spread to others. The choice between topical and oral antibiotics depends on the severity and extent of the infection.
- Topical Antibiotics: For mild cases of impetigo, a topical antibiotic cream or ointment applied directly to the sores can be effective. This localized treatment minimizes the infection while reducing the risk of spreading the bacteria.
- Oral Antibiotics: More widespread or severe cases may require oral antibiotics. These systemic treatments help eliminate the bacteria from inside the body, addressing both visible symptoms and asymptomatic bacterial carriers.
The Importance of Completing Prescribed Treatments
Complete the full course of prescribed antibiotics, even if symptoms improve before finishing the medication. This action fully eradicates the infection and prevents the development of antibiotic-resistant bacteria, making future outbreaks easier to treat.
In conclusion, understanding how impetigo is transmitted helps prevent its spread. Practice good hygiene, seek early treatment, and educate others. Together, we can protect vulnerable populations and reduce impetigo outbreaks.




